Duck Creek Claims
Intelligent Claims Execution When and Where It Matters Most
Duck Creek Claims is a modern P&C insurance claims management
software platform built to help carriers resolve claims faster, more
accurately, and with greater control.
As an enterprise‑grade claims management system fully integrated with
policy and billing, it automates the end‑to‑end claims lifecycle —from
FNOL to settlement— using configurable workflows and AI‑enabled decision support.
Built on Duck Creek’s Intelligent Core, it helps insurers improve cycle times, optimize reserves, strengthen fraud detection, and reduce manual effort across personal and complex commercial lines.
Trusted By


Claims Management, Reimagined
Claims are where moments of truth happen—for policyholders and insurers alike. But complex processes, manual steps, and fragmented systems can slow resolution, obscure financial visibility, and put pressure on both service and outcomes.
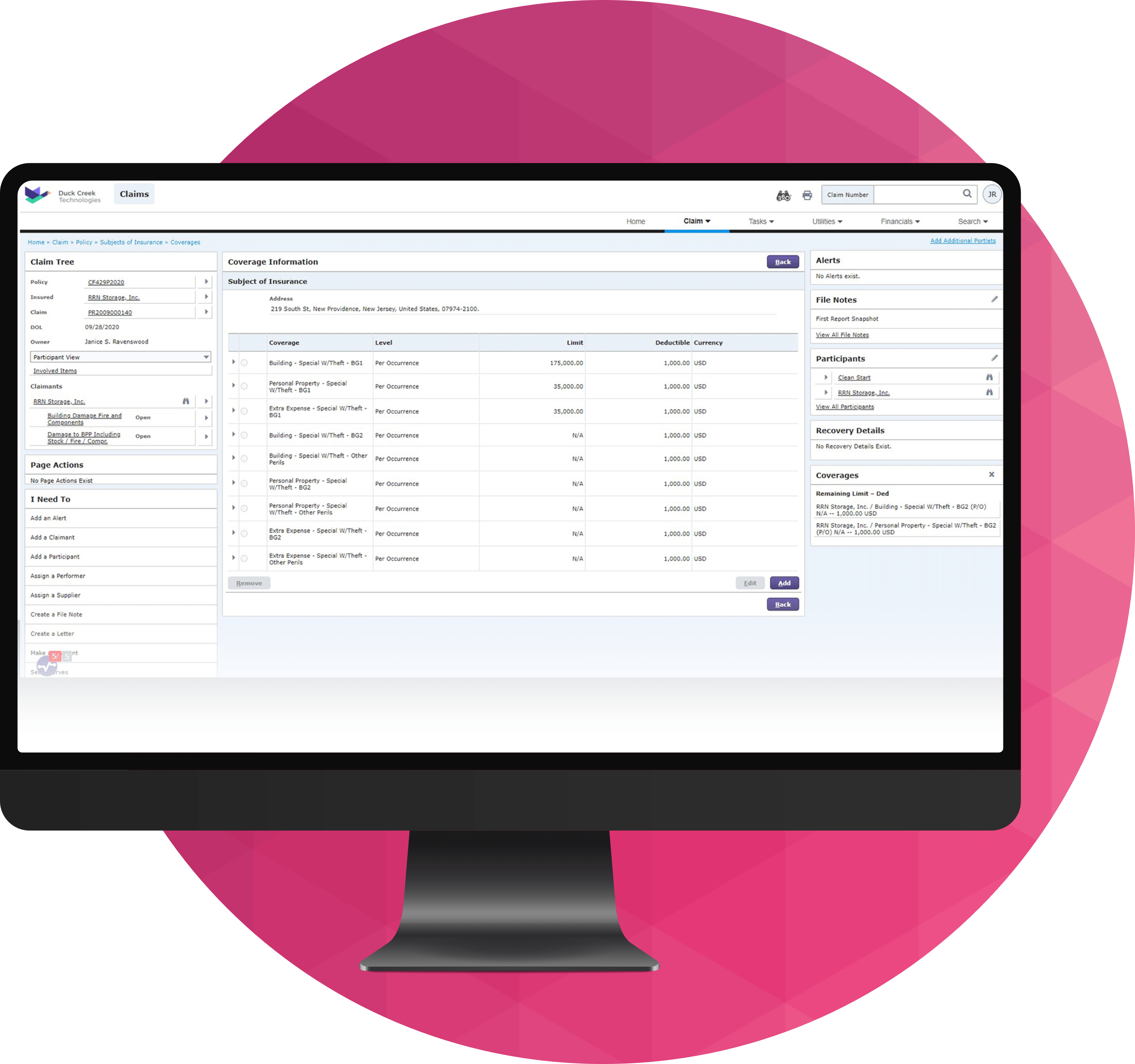
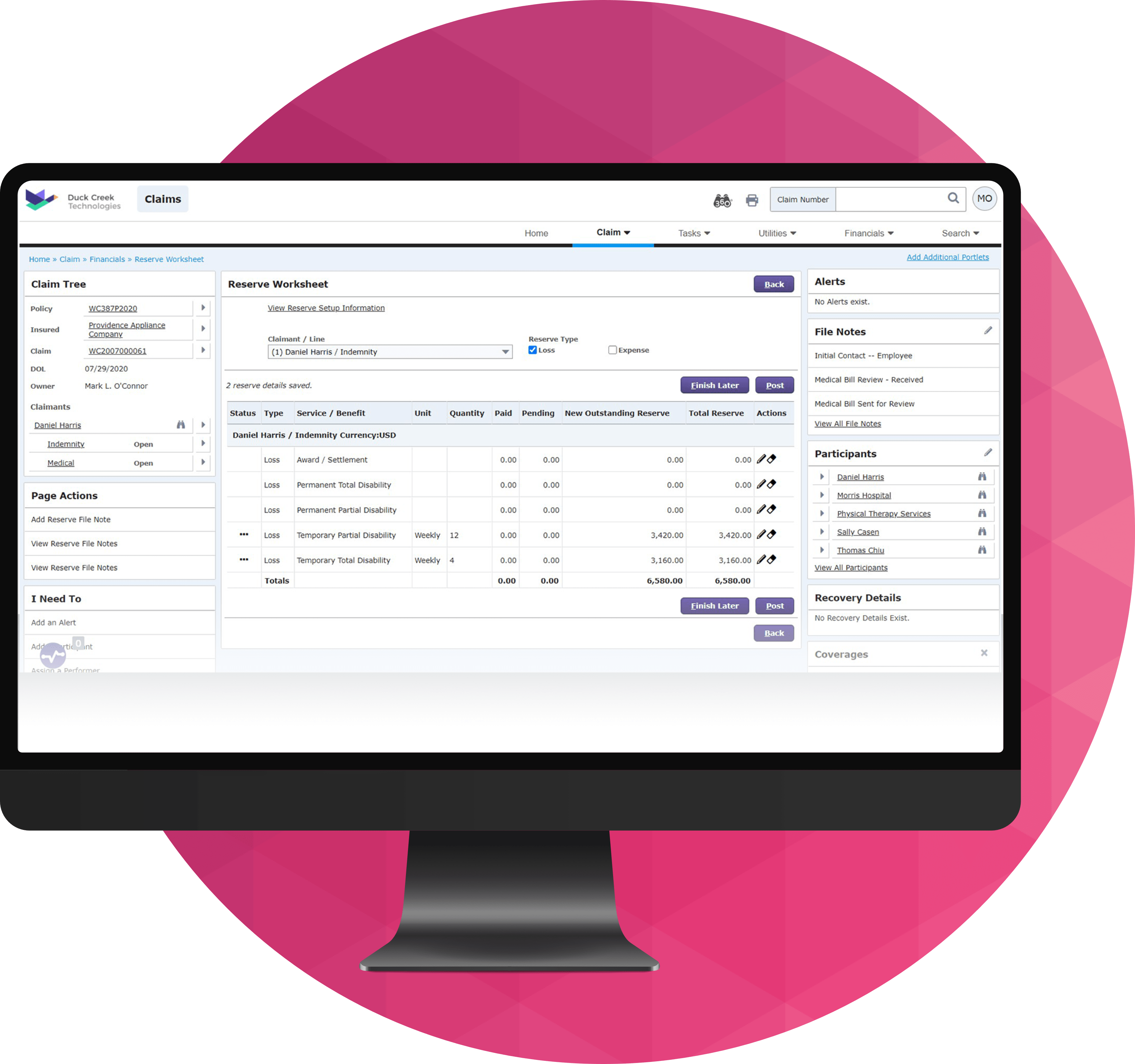
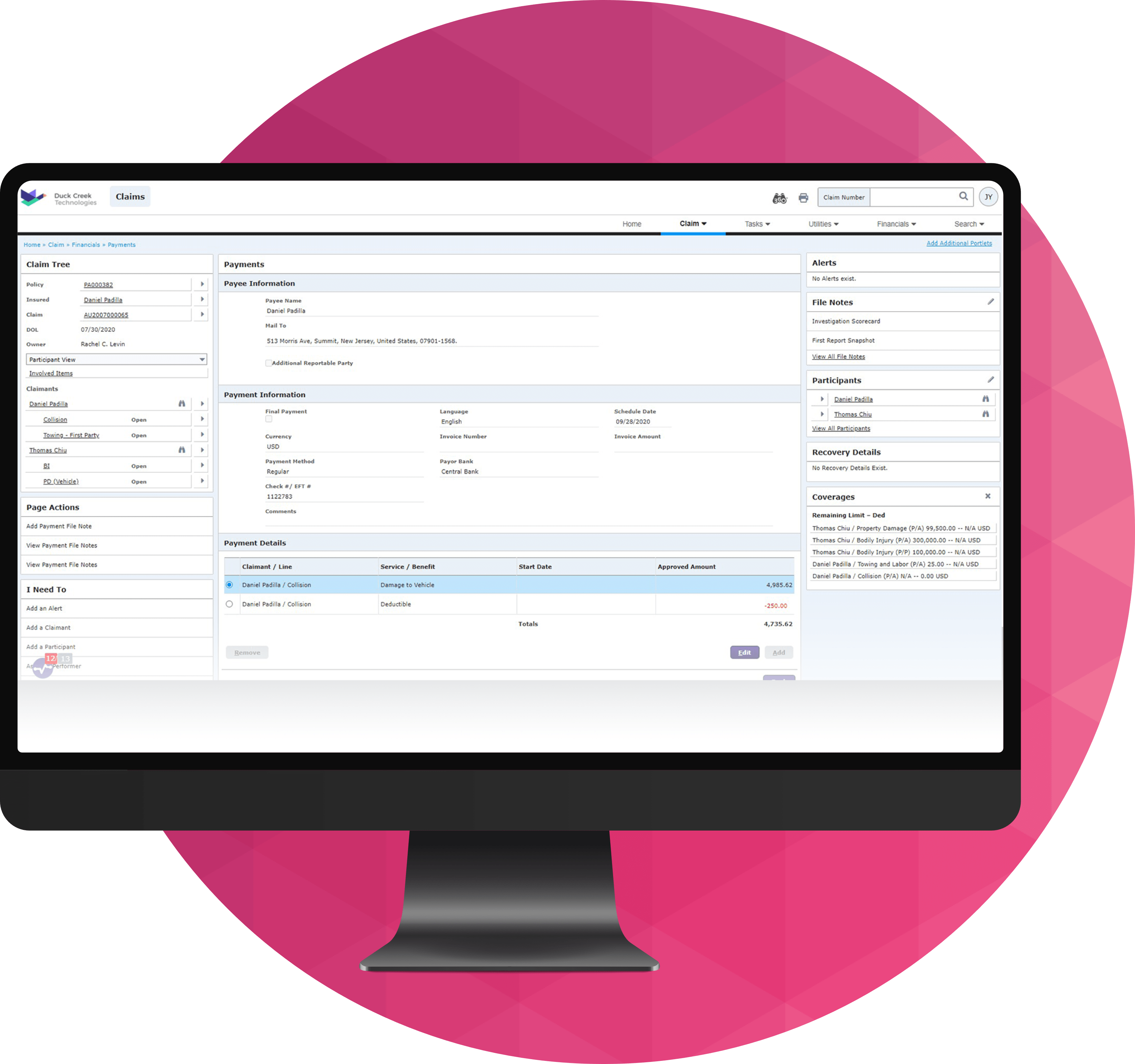
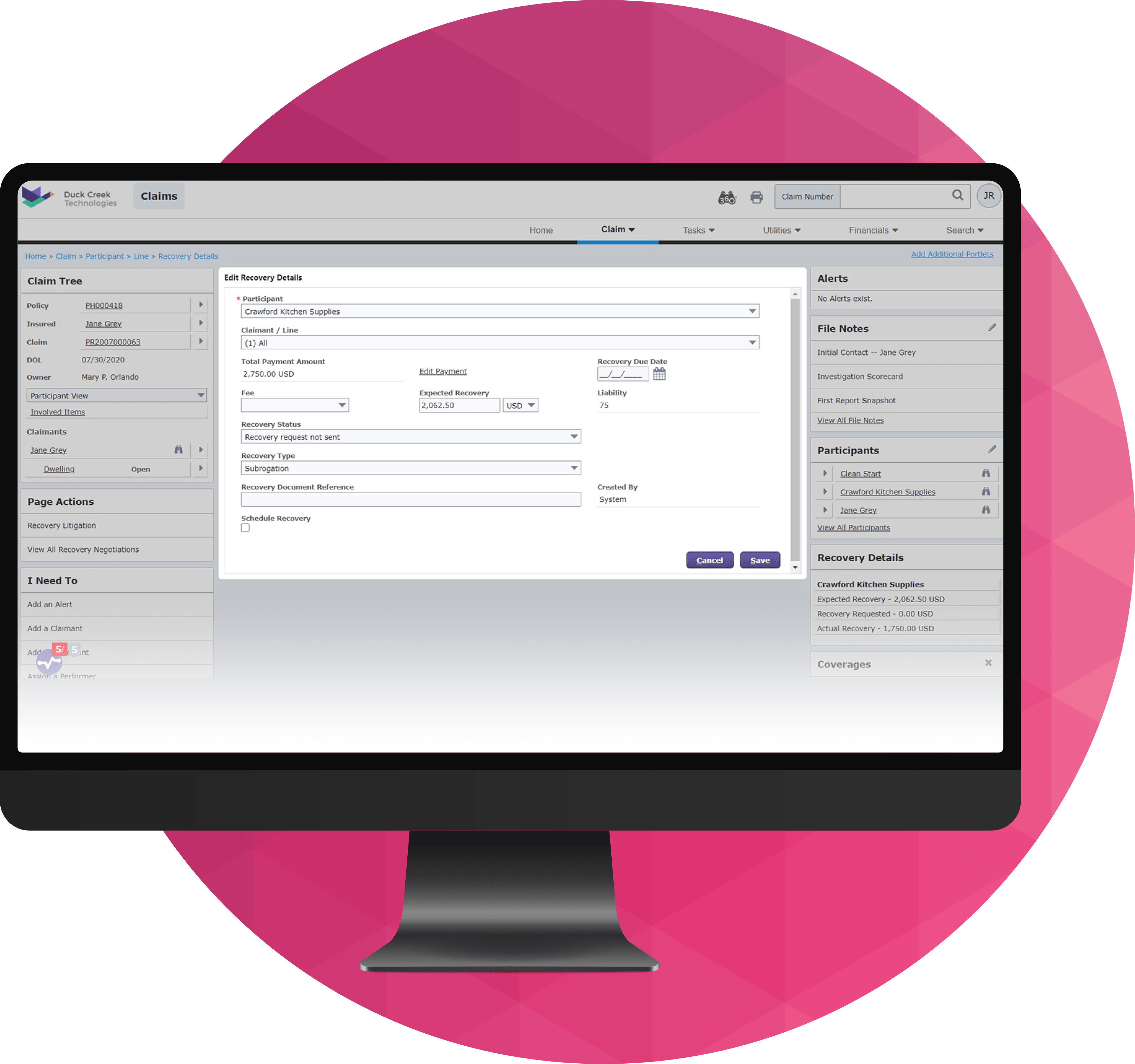
Duck Creek Claims reimagines the claims lifecycle from first notice of loss (FNOL) to settlement and subrogation.
Built for P&C insurers and powered by insurance‑specific AI, it automates workflows, enables intelligent triage and fraud detection, and delivers real‑time claims and financial visibility through Duck Creek Clarity. Fully integrated with policy, billing, and partner ecosystems, Duck Creek Claims reduces manual effort, supports personal and complex commercial claims, and provides transparent, audit‑ready control—so carriers can resolve claims faster and deliver better outcomes for everyone involved.
Explore how insurers modernize claims for faster, more accurate outcomes.
Why Duck Creek Claims
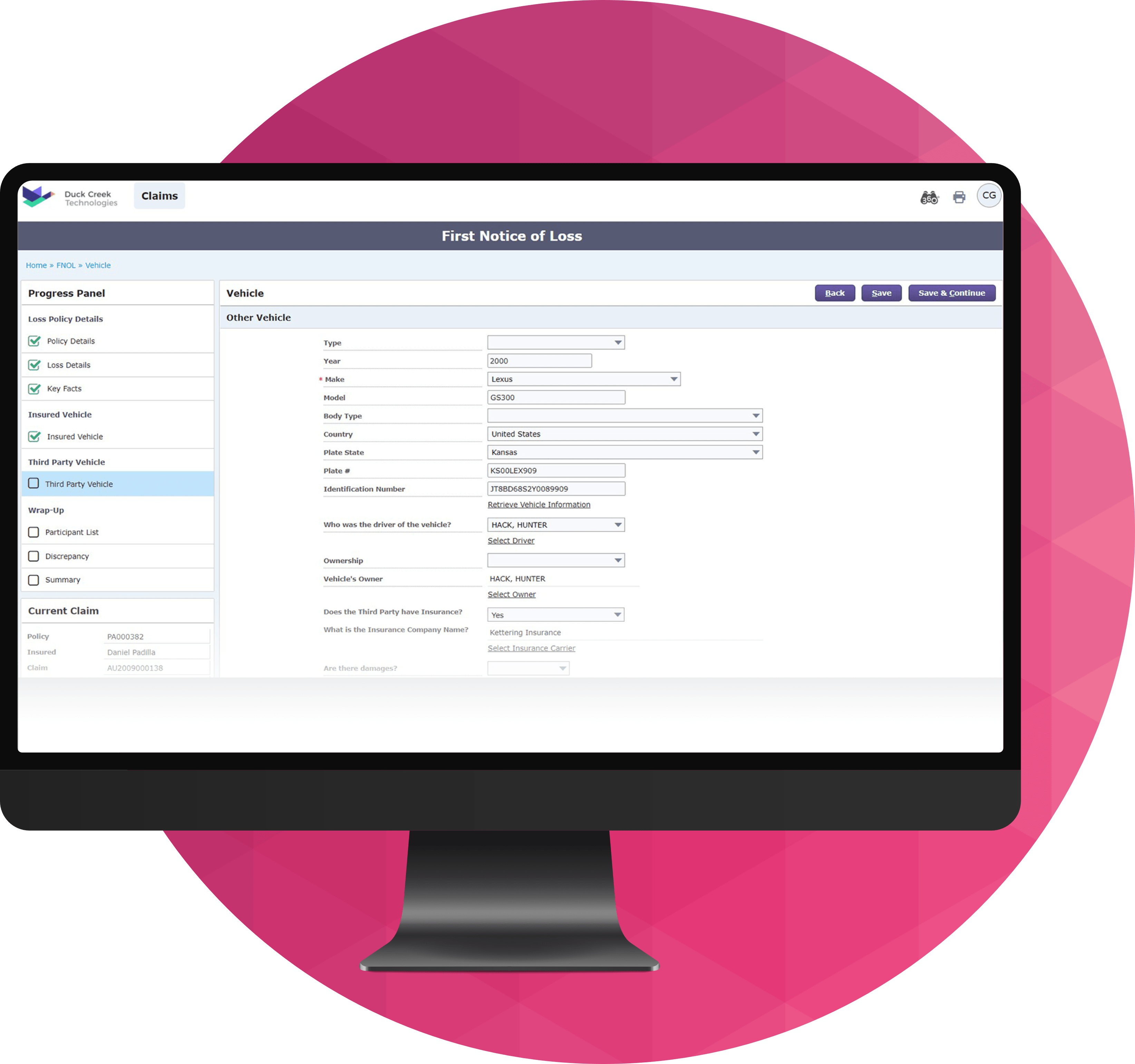
Reduce Claims Management Cycle Times
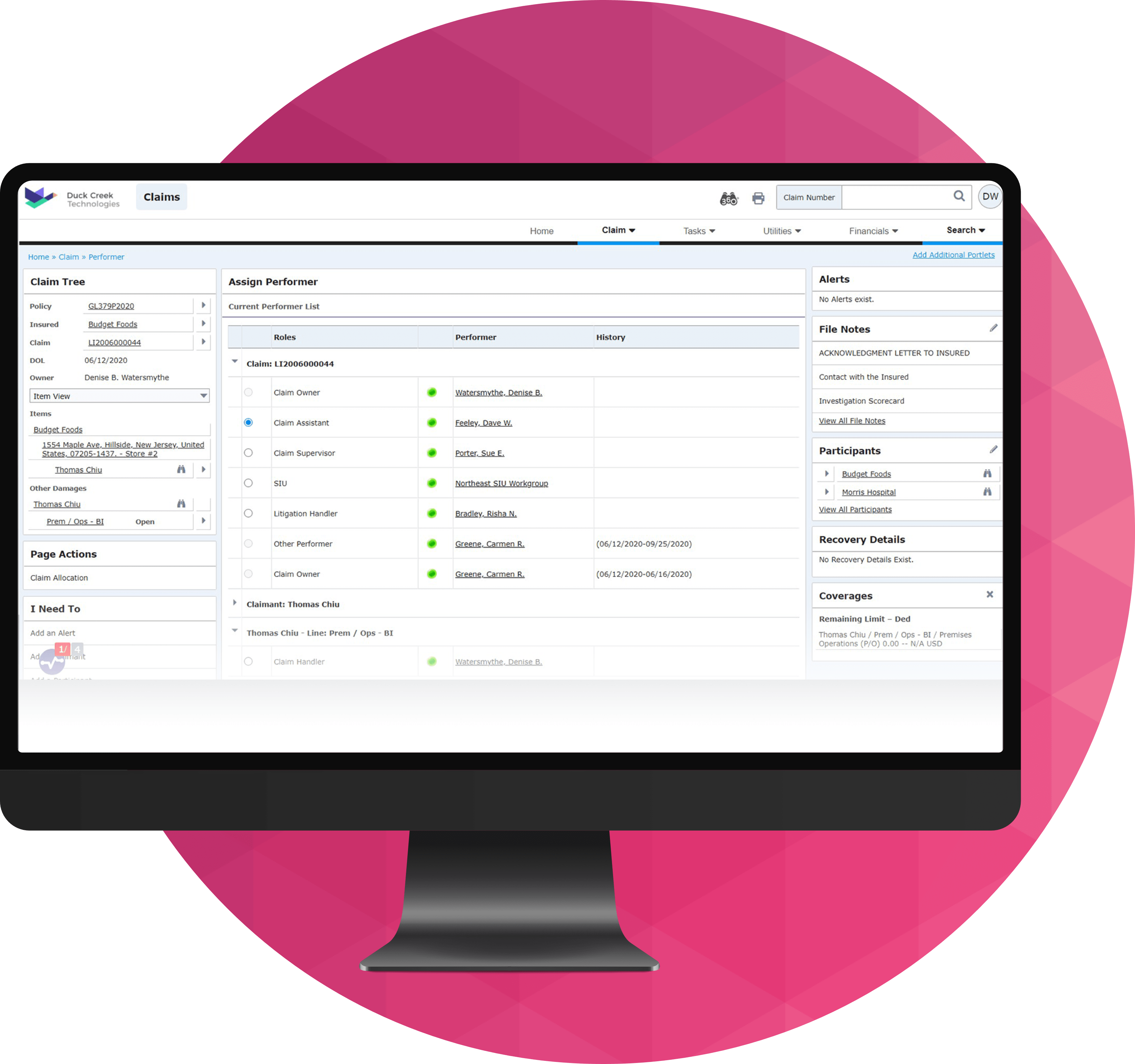
Streamline FNOL, triage, and assignment with guided workflows, data enrichment, and agentic orchestration that prioritize high-risk cases and shorten time-to-settlement.
Increase Customer Satisfaction
Deliver transparent, omnichannel communications, faster payouts through embedded payments, and proactive claim updates, improving policyholder trust and NPS.
Innovate Faster & Improve Efficiencies
Leverage continuous SaaS updates, low-code configuration, open APIs, and Clarity dashboards for real-time KPIs so teams iterate faster, lower cost-per-claim, and scale without adding headcount.
Insurers’ Go-to SaaS Claims Management System
30 Million+
Claims processed via Duck Creek OnDemand
<1
Days to make an assignment or claims workflow rule change
60,000+
Claims per day has scaled to during a CAT event
Claims Features
What Our Customers Say
“Moving our systems to a cloud-native, continuously updated, highly-secure system with Duck Creek is a transformative step in our journey to a model that will ensure we remain meaningful and competitive in our marketplace.”
Adam Solomon
Chief Information Officer, Mutual Benefit Group
What Analysts Say about Duck Creek
Duck Creek named a luminary in Celent Claims Systems Vendors: North America P&C Insurance.
Duck Creek offers a top-tier, leading-edge claims system that caters to insurers of all lines of business and complexity levels, enabling insurers to optimize claims processes, enhance customer satisfaction, and achieve cost savings. Their exceptional claims system, along with their ongoing commitment to providing exceptional technology solutions, solidifies Duck Creek’s position as a top performer in the industry.
Karlyn Carnahan, Head of Insurance, Celent
Partner Ecosystem Integrations
Discover the comprehensive partner ecosystem that Duck Creek Claims offers, featuring numerous integrations with technology providers specializing in different claims lifecycle use cases.








Frequently Asked Questions
Duck Creek is committed to providing the information you need to solve your insurtech needs. Find answers to common questions below or, if this information isn’t enough, fill out the form at the bottom of the page. Our team will respond with the answers you need.
Can Duck Creek Claims support a low‑touch or no‑touch claims experience?
Yes. Duck Creek Claims supports low‑touch and no‑touch claims experiences by combining configurable business rules, straight‑through processing, and automated decisioning across the claims lifecycle. Low‑complexity claims can be automatically triaged, adjudicated, and paid—while higher‑complexity cases are seamlessly routed to adjusters with the right context and controls.
As part of an Intelligent Core used by insurers globally, Duck Creek Claims enables consistent, customer‑centric claims experiences across markets. Carriers can tailor automation levels by product, region, or loss type—delivering faster resolutions and improved customer satisfaction without sacrificing oversight or compliance.
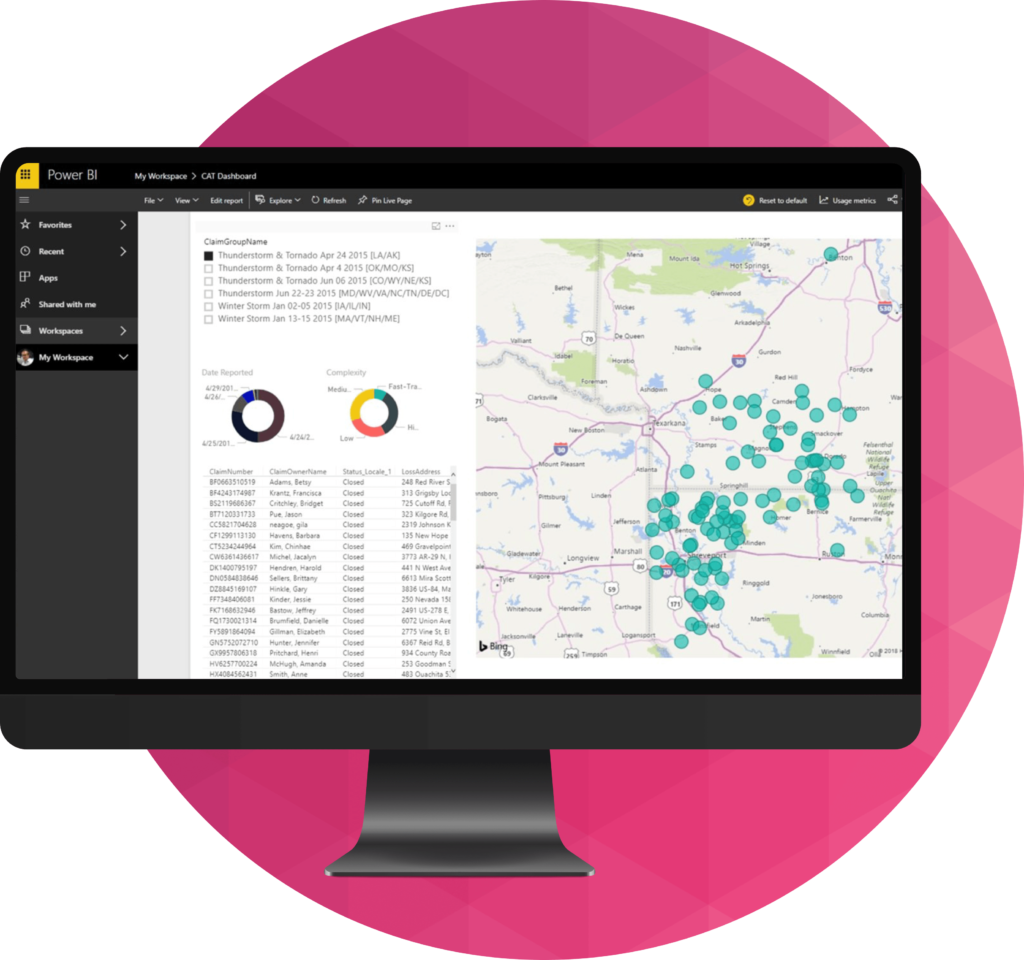
How does the system handle high‑volume CAT (catastrophe) management?
Duck Creek Claims is designed to remain resilient during high‑volume CAT events by leveraging cloud‑native scalability, automated workflows, and configurable business rules. Delivered through Duck Creek OnDemand, the platform can elastically scale to handle sudden spikes in claim volume—without manual intervention or system degradation.
Built on an Intelligent Core engineered for operational continuity, Duck Creek Claims enables carriers to maintain service levels during catastrophic events across regions and markets. Automated intake, prioritization, and assignment help carriers respond faster when it matters most—while ensuring claims data remains accurate, auditable, and accessible throughout the event lifecycle.
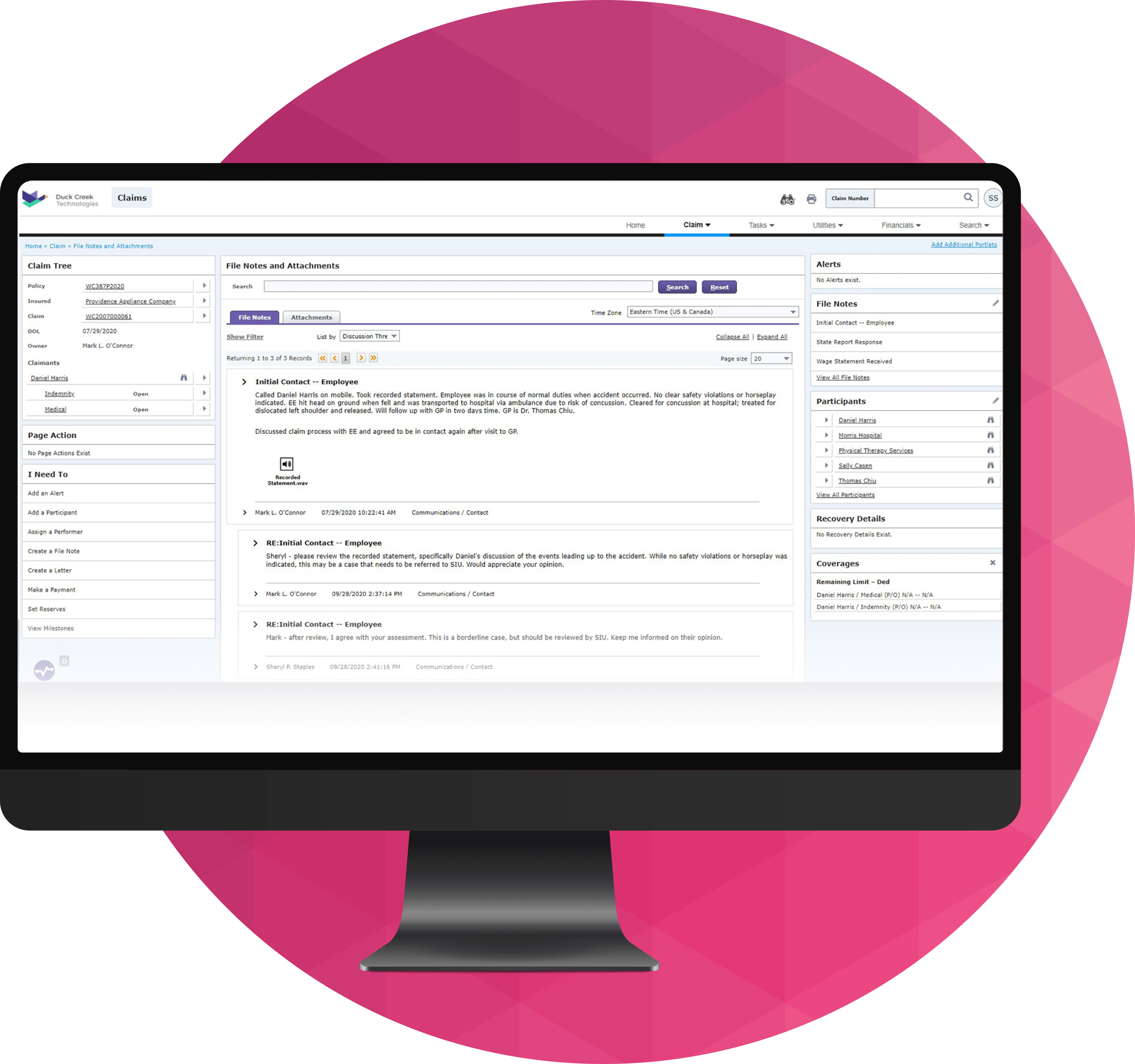
How does Duck Creek Claims enable faster, more accurate claims decisions?
Duck Creek Claims enables faster, more accurate claims decisions by combining real‑time data access, configurable business rules, and embedded intelligence across the claims lifecycle. From FNOL through settlement, the system surfaces the right information at the right moment—supporting automated decisions for low‑complexity claims while guiding adjusters through more nuanced scenarios.
Because these decisioning capabilities are embedded within an Intelligent Core used by insurers globally, Duck Creek Claims ensures consistency, transparency, and control across products, regions, and regulatory environments. Insurers can improve cycle times, reduce leakage, and deliver better customer experiences—without relying on disconnected tools or manual workarounds.
To explore how embedded intelligence helps insurers modernize claims operations and drive better outcomes, read more here:
Explore faster, more accurate decisions with Duck Creek Claims Intelligence